Nonmelanoma Skin Cancers
Frequently Asked Questions
What are nonmelanoma skin cancers?
Nonmelanoma skin cancers are cancers that arise from cells in the outer layers of the skin but do not involve melanocytes (the pigment-producing cells affected in melanoma). The two most common types are basal cell carcinoma (BCC), which originates from basal cells at the bottom of the epidermis, and squamous cell carcinoma (SCC), which develops from squamous cells in the outer epidermis. BCC is the most frequent form of skin cancer and typically grows slowly, while SCC has a higher risk of spreading if left untreated.
What are the warning signs of basal cell carcinoma and squamous cell carcinoma?
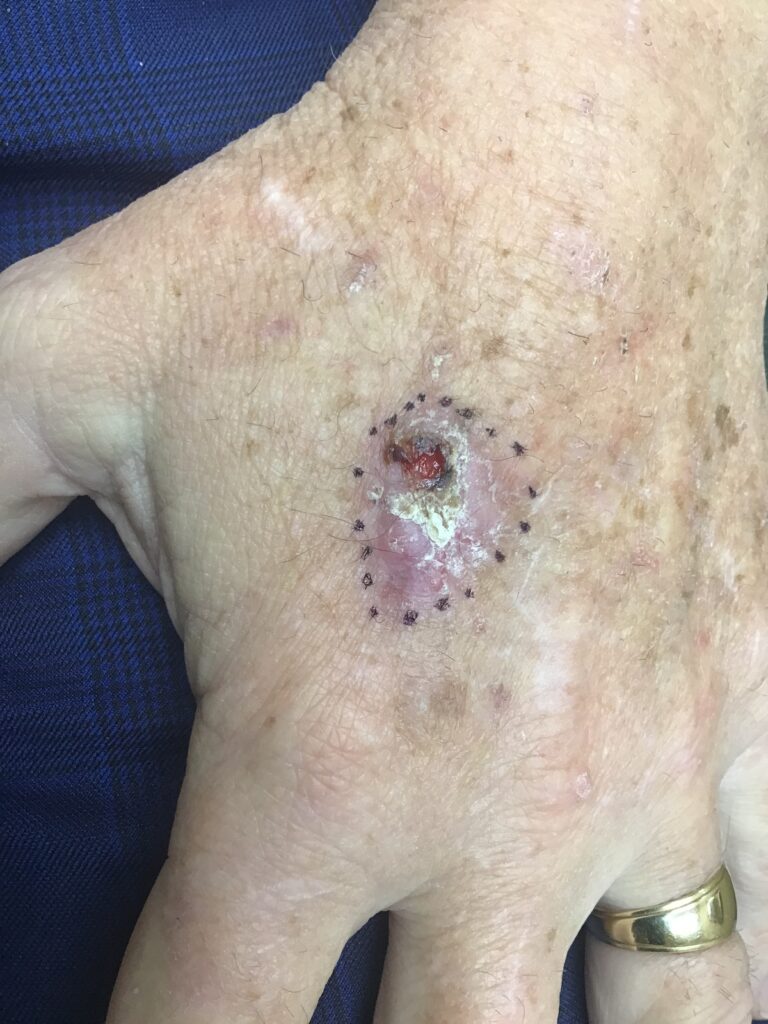
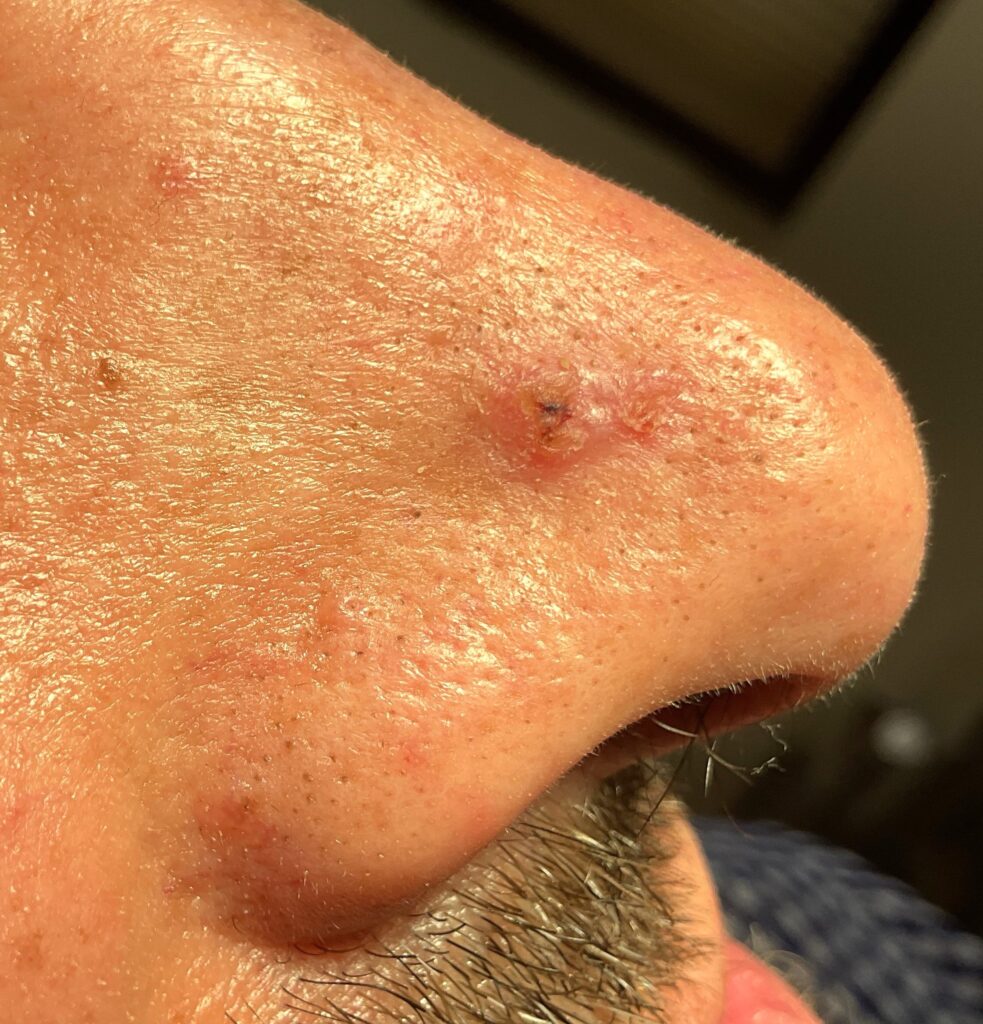
Common warning signs include a persistent sore that does not heal or repeatedly bleeds and crusts, a pearly or translucent bump (often a sign of BCC), a scaly rough patch or raised red nodule (often a sign of SCC), a scar-like area of thickened skin with poorly defined borders, and tenderness, pain, or itching in a suspicious spot. Nonmelanoma skin cancers often develop on sun-exposed areas of the body, including the face, ears, scalp, neck, hands, forearms, and lower legs.
What causes nonmelanoma skin cancers?
Chronic ultraviolet (UV) exposure from the sun and tanning beds is the leading cause of nonmelanoma skin cancers. Other risk factors include having fair skin with freckles, blond or red hair, and light eyes, a history of severe blistering sunburns (especially during childhood), being over 50 years of age, having a personal or family history of skin cancer, taking immunosuppressive medications, and chronic exposure to radiation, arsenic, or industrial chemicals.
What is Mohs micrographic surgery and when is it used?
Mohs micrographic surgery is considered the gold standard for treating high-risk nonmelanoma skin cancers or those in cosmetically sensitive areas such as the face, ears, and scalp. This technique allows for the precise removal of cancer while sparing as much healthy tissue as possible. Each layer is examined immediately under the microscope until the margins are clear, resulting in the highest cure rate and best cosmetic outcomes for basal cell carcinoma and squamous cell carcinoma.
What is the difference between basal cell carcinoma and squamous cell carcinoma?
Basal cell carcinoma is the most common type of skin cancer and typically grows slowly, rarely spreading to distant organs, though it can be locally destructive if left untreated. Squamous cell carcinoma is the second most common skin cancer and has a higher risk of metastasizing (spreading), particularly if left untreated or arising in high-risk areas such as the lips or ears. Both types develop on sun-exposed areas and require prompt treatment for the best outcomes.
Can nonmelanoma skin cancers be prevented?
Yes, prevention starts with protecting your skin from UV damage. Apply broad-spectrum SPF 30 or higher sunscreen to all exposed skin during outdoor activities, wear protective clothing including wide-brimmed hats and long sleeves, avoid peak sun hours between 10am and 4pm, never use tanning beds, schedule annual full-body skin checks with a dermatologist, perform monthly self-examinations at home, and report any new, changing, or non-healing spots to your dermatologist promptly.
What is the prognosis for nonmelanoma skin cancers?
The outlook for nonmelanoma skin cancers is generally excellent when detected early. Most basal cell carcinomas and squamous cell carcinomas are curable, especially with timely intervention. However, delaying treatment can lead to significant local tissue destruction, disfigurement, and in the case of squamous cell carcinoma, potential spread to other organs. Regular skin checks and early evaluation of suspicious lesions are critical for the best outcomes.